Rosacea affects over 415 million people worldwide, yet conventional dermatology still treats it primarily as a vascular skin condition — prescribing topical antibiotics, azelaic acid, and laser therapy. These treatments can reduce visible symptoms, but they do nothing to address why the immune system is chronically overreacting in the first place. The answer, increasingly, lies in the gut.
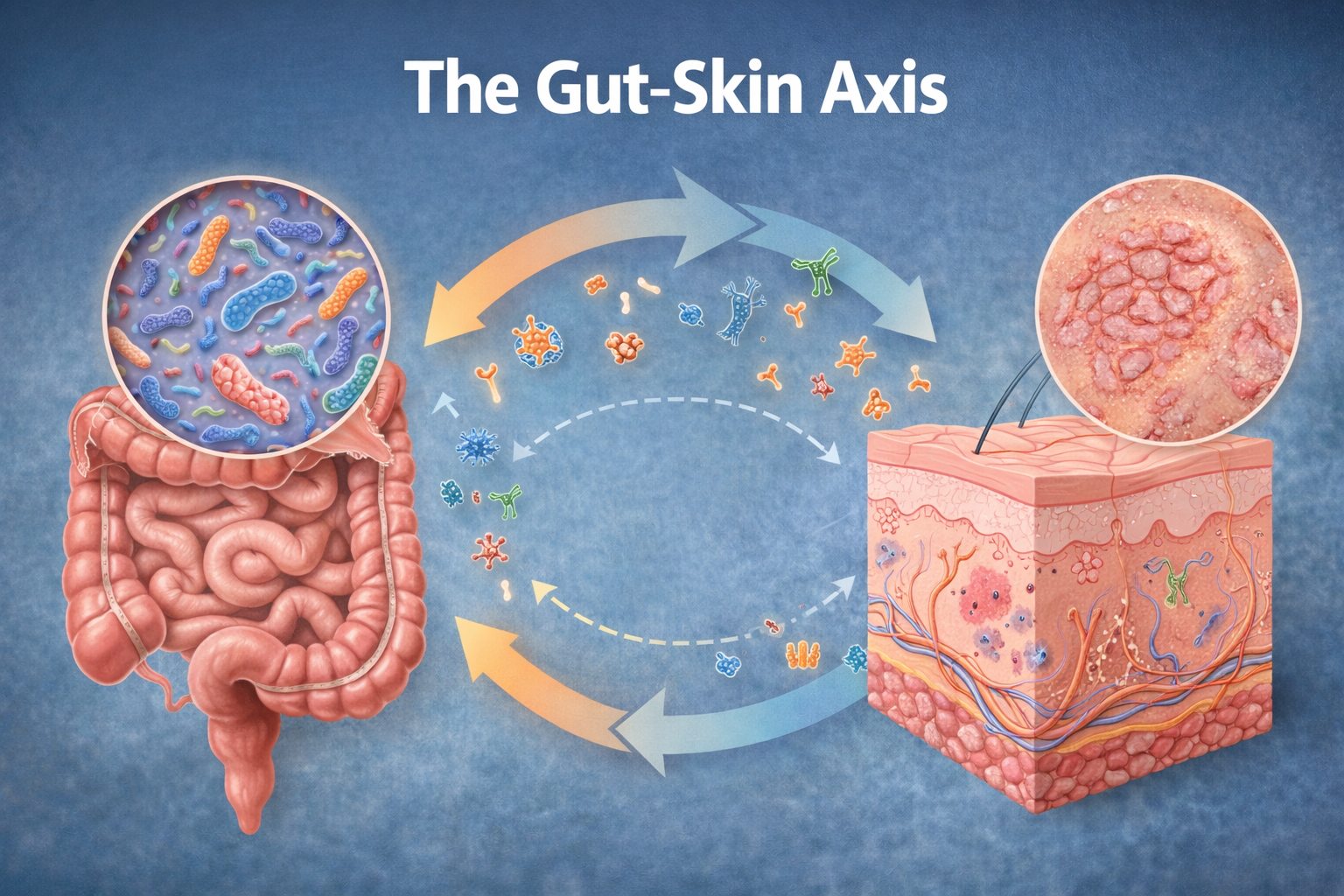
The Rosacea-Gut Connection: What the Research Shows
A landmark 2008 study published in the Journal of the American Academy of Dermatology found that rosacea patients had a dramatically higher prevalence of small intestinal bacterial overgrowth (SIBO) compared to healthy controls — 46% vs 5%. When SIBO was treated with antibiotics, rosacea symptoms improved significantly in 96% of patients. This was a pivotal finding: rosacea is not just a skin condition. It is a manifestation of gut dysfunction.
“The skin is a window into the gut. When the gut is inflamed, the skin reflects it. Rosacea is one of the clearest examples of this principle.”
— Dr. Alan Logan, The Clear Skin Diet
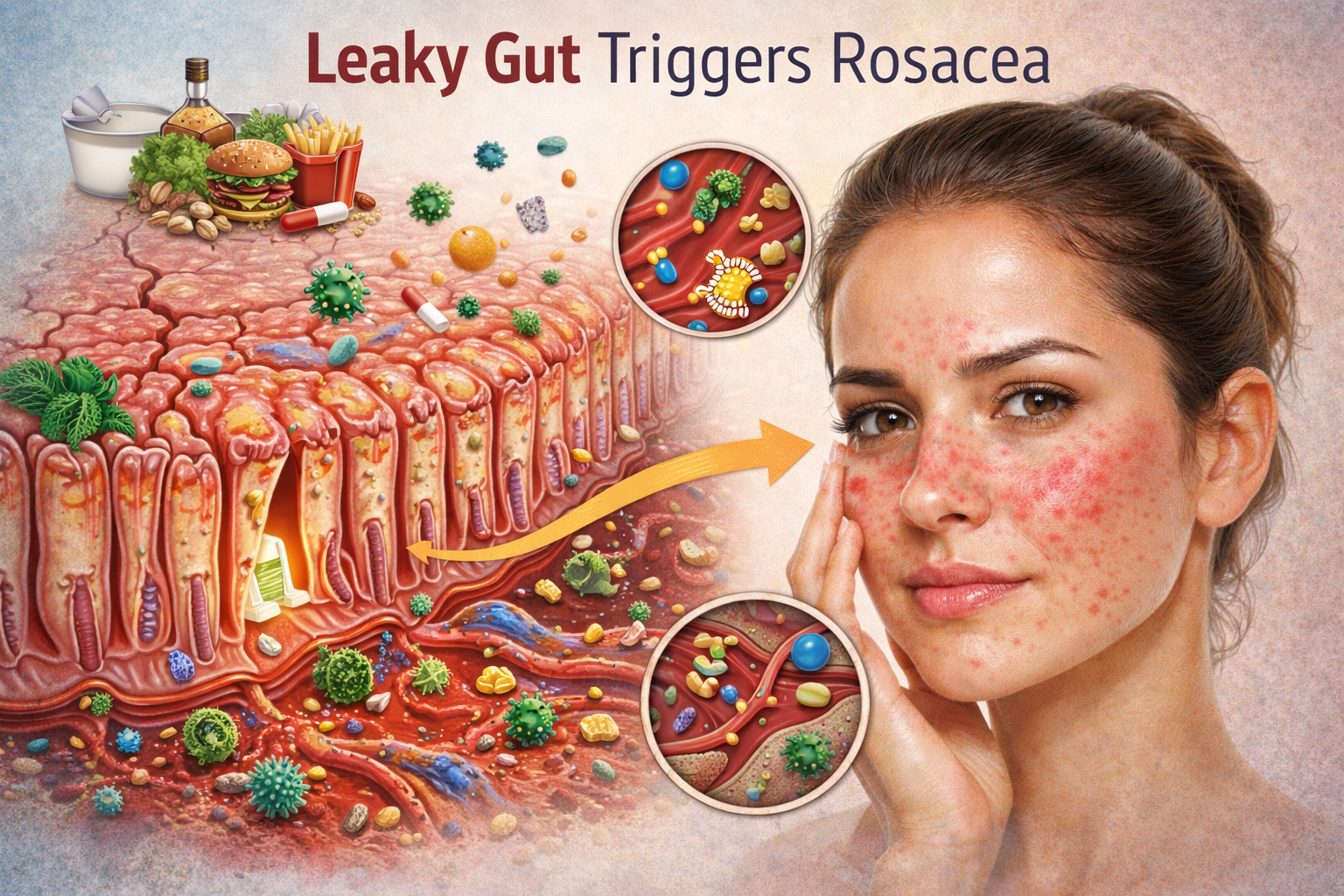
How Leaky Gut Triggers Facial Flushing
The mechanism connecting leaky gut to rosacea involves several interconnected pathways. When intestinal permeability is increased, bacterial toxins (particularly lipopolysaccharides from gram-negative bacteria) enter the bloodstream. These LPS molecules trigger a powerful immune response, activating toll-like receptor 4 (TLR4) on immune cells throughout the body.
In the skin, TLR4 activation triggers the release of cathelicidin antimicrobial peptides — specifically LL-37. In healthy skin, LL-37 is a normal part of the immune defense. In rosacea patients, LL-37 is overproduced and abnormally processed, leading to the characteristic vasodilation, inflammation, and flushing of rosacea.
The SIBO-Rosacea Connection
Small intestinal bacterial overgrowth (SIBO) occurs when bacteria that normally live in the large intestine migrate into the small intestine, where they ferment carbohydrates and produce hydrogen and methane gas. This creates bloating, gas, and — critically — increased intestinal permeability.
- Bloating and gas, especially after carbohydrate-rich meals
- Rosacea that worsens after eating fermentable foods (onions, garlic, beans, wheat)
- Rosacea that improved during or after antibiotic treatment
- History of food poisoning or gastroenteritis before rosacea onset
- Constipation or diarrhea alongside skin flares
The Histamine Connection
Many rosacea patients are also histamine intolerant. Certain gut bacteria produce histamine as a metabolic byproduct, and when the gut lining is permeable, this histamine enters the bloodstream and triggers the vasodilation and flushing characteristic of rosacea. Foods high in histamine — fermented foods, aged cheeses, wine, processed meats — are classic rosacea triggers for this reason.
Practical Note: If your rosacea worsens after eating fermented foods, aged cheeses, or drinking wine, histamine intolerance may be a significant factor. Consider a low-histamine diet trial alongside gut healing protocols.
The Protocol: Healing Leaky Gut for Rosacea
- Phase 1 — Remove: Eliminate gluten, dairy, alcohol, refined sugar, and high-histamine foods for 30 days
- Phase 2 — Repair: L-glutamine (5g daily), zinc carnosine (75mg daily), collagen peptides (10g daily)
- Phase 3 — Repopulate: High-CFU probiotic with Lactobacillus rhamnosus GG and Bifidobacterium strains
- Phase 4 — Rebalance: Quercetin (500mg daily) as a natural antihistamine and mast cell stabilizer
- Ongoing: Omega-3 fish oil (3g daily) to reduce systemic inflammation and support skin barrier
Rosacea is one of the skin conditions most responsive to gut healing. Many people in our community have achieved complete remission by addressing intestinal permeability, SIBO, and histamine intolerance — without any topical treatments. It takes time and consistency, but the results can be transformative.